
Breast Thermography: Accurate breast cancer risk assessment with thermal imaging
|
Breast Thermography: Is It Underutilized?
 The FDA published information in Journal Watch in June of 2011 that is packed with presumptive and incorrect information about breast thermography and they have to know it! Breast thermography was approved in 1982 as an adjunct to mammography to evaluate for breast cancer. In 2004 the FDA rejected breast thermography as a stand alone test for breast cancer screening by a vote of 5-4. Three of the members voting against it had a conflict of interest because of ties to the mammography industry.
The FDA published information in Journal Watch in June of 2011 that is packed with presumptive and incorrect information about breast thermography and they have to know it! Breast thermography was approved in 1982 as an adjunct to mammography to evaluate for breast cancer. In 2004 the FDA rejected breast thermography as a stand alone test for breast cancer screening by a vote of 5-4. Three of the members voting against it had a conflict of interest because of ties to the mammography industry.
Nonetheless Helen Barr, MD, the director of the Division of Mammography Quality and Radiation Programs in the FDA's Center for Devices and Radiological Health stated, "While there is plenty of evidence that mammography is effective in breast cancer detection, there is simply no evidence that thermography can take its place." Come on, Dr. Barr, keep up with the current and the old literature on this much needed test!
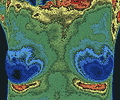 The greatest loss of life from breast cancer occurs betweeen the ages of 30 and 50. Fortunatly, women today have more options availble to them to help in the detection of breast cancer than in the past decades. Unfortunarly, education and awereness of these options, and their effectiveness in detecting breast cancer at different stages in life, are woefully deficient.
The greatest loss of life from breast cancer occurs betweeen the ages of 30 and 50. Fortunatly, women today have more options availble to them to help in the detection of breast cancer than in the past decades. Unfortunarly, education and awereness of these options, and their effectiveness in detecting breast cancer at different stages in life, are woefully deficient.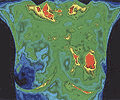 This thermal imaging technology has been validated as effective and approved by the FDA for breast cancer risk assessment. Recent studies have documented that thermography, as a single test, has 99% accuracy in identifying breast cancer in women in the 30 to 55 age group. For women over 55 the accuracy is still an impressive 95%.
This thermal imaging technology has been validated as effective and approved by the FDA for breast cancer risk assessment. Recent studies have documented that thermography, as a single test, has 99% accuracy in identifying breast cancer in women in the 30 to 55 age group. For women over 55 the accuracy is still an impressive 95%.

